Journal Description
Trauma Care
Trauma Care
is an international, peer-reviewed, open access journal on traumatic injury and psychological trauma published quarterly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 21 days after submission; acceptance to publication is undertaken in 3.5 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
- Companion journal: Healthcare.
Latest Articles
Community Participation Trajectories over the 5 Years after Traumatic Brain Injury in Older Veterans: A U.S. Veterans Affairs Model Systems Study
Trauma Care 2024, 4(2), 174-188; https://doi.org/10.3390/traumacare4020014 - 14 May 2024
Abstract
►
Show Figures
Background: Given the aging of the overall U.S. population, the resulting changes in healthcare needs especially among veterans, and the high prevalence of traumatic brain injury (TBI) among older adults, additional research is needed on community participation after TBI in older veterans. The
[...] Read more.
Background: Given the aging of the overall U.S. population, the resulting changes in healthcare needs especially among veterans, and the high prevalence of traumatic brain injury (TBI) among older adults, additional research is needed on community participation after TBI in older veterans. The current study examined predictors of community participation trajectories over the 5 years after TBI in veterans who were 55 years of age or older upon injury. Method: This study included data from 185 participants in the U.S. Department of Veterans Affairs TBI Model System national study who had sustained a TBI at age 55 or older and had completed at least one of each Participation Assessment with Recombined Tools-Objective (PART-O) subscale scores at one or more follow-up time points (1, 2, and 5 years post-TBI). Results: PART-O Productivity, Social, and Out and About scores remained constant over time. Lower PART-O Productivity trajectories were seen among participants who were unemployed at the time of injury (p = 0.023). Lower PART-O Social trajectories were seen among participants who had a lower education level (p = 0.021), were unmarried at injury (p < 0.001), and had private insurance coverage (p < 0.033). Conclusion: These findings add to the growing body of literature on TBI and community participation by focusing on an older adult veteran population. There is an urgency to understand the needs of this group, many of whom are aging with service-connected disabilities including TBI. Veterans with characteristics identified herein as being associated with lower community participation trajectories would be prime candidates for interventions that aim to increase community and social engagement after later-life TBI.
Full article
Open AccessCommunication
A Network Analysis of Symptoms of Post-Traumatic Stress Disorder and Facets of Mindfulness
by
Mikael Rubin
Trauma Care 2024, 4(2), 167-173; https://doi.org/10.3390/traumacare4020013 - 8 May 2024
Abstract
►▼
Show Figures
Post-traumatic Stress Disorder (PTSD) is a mental health concern impacting a large proportion of the population. There is a growing interest in mindfulness-based treatments for PTSD. However, some individuals with PTSD do not respond to treatment. Identifying factors that may provide a more
[...] Read more.
Post-traumatic Stress Disorder (PTSD) is a mental health concern impacting a large proportion of the population. There is a growing interest in mindfulness-based treatments for PTSD. However, some individuals with PTSD do not respond to treatment. Identifying factors that may provide a more precise treatment approach has the potential to enhance response. Network analysis is a data-driven methodology that has been used to suggest specific targets for treatment. To date, there has not been a network analysis examining the interrelation between PTSD symptoms and trait mindfulness. The current study is an exploratory analysis of N = 214 adults from a non-clinical sample who endorsed a Criterion A traumatic event and completed the PTSD Checklist for DSM-5 and the Five Facet Mindfulness Questionnaire. Both undirected and directed networks were generated to identify links between PTSD symptom clusters and the facets of mindfulness. Both networks highlighted the connection between the PTSD symptom cluster Alterations in Arousal and Reactivity and the Awareness facet of mindfulness; and the PTSD symptom cluster Negative Alterations in Cognitions and Mood with the Non-judging facet of mindfulness. Taken together, these findings provide further evidence that greater mindfulness is generally associated with lower PTSD symptoms. Importantly, the findings highlight Non-judgement and Awareness as facets that might warrant further investigation in the context of mindfulness-based treatment efforts for PTSD.
Full article

Figure 1
Open AccessReview
Skin Substitutes: Filling the Gap in the Reconstructive Algorithm
by
Pedro Fuenmayor, Gustavo Huaman, Karla Maita, Kelly Schwemmer, Wes Soliman, Sahar Abdelmoneim, Stephanie Pintos, Mark Dickinson, Edward Gonzalez and Ricardo Castrellon
Trauma Care 2024, 4(2), 148-166; https://doi.org/10.3390/traumacare4020012 - 3 May 2024
Abstract
►▼
Show Figures
Background: Skin substitutes play a crucial role in wound care by actively modulating the wound healing process, promoting angiogenesis, and protecting the integrity of the native extracellular matrix. Consequently, surgeons have increasingly recognized these resources as excellent complements to improve reconstructive outcomes. This
[...] Read more.
Background: Skin substitutes play a crucial role in wound care by actively modulating the wound healing process, promoting angiogenesis, and protecting the integrity of the native extracellular matrix. Consequently, surgeons have increasingly recognized these resources as excellent complements to improve reconstructive outcomes. This review focuses on the author’s experience using these biomaterials in complex cases, highlighting the benefits they bring to patient care. Methods: A literature review was conducted to evaluate the regenerative properties of skin substitutes and their applicability in head and neck, upper and lower extremities, and trunk reconstruction. Results: The reviewed literature, along with the authors’ experience, supports the adjunct use of skin substitutes in various reconstructive situations. Combining them with skin grafts improves resulting skin quality and may also enhance donor site healing. They have proven to be effective in addressing chronic venous ulcers, traumatic wounds with limited donor tissues for coverage, extensive burns, diabetic foot ulcers, and oncological resections in the face and scalp. Furthermore, combining them with autologous tissue shows promising results in achieving stable closure. Conclusions: Incorporating skin substitutes in complex reconstructive scenarios offers multiple benefits. Their regenerative properties and ability to modulate the healing process contribute to enhanced outcomes and reduced overall costs.
Full article

Figure 1
Open AccessFeature PaperArticle
Legal Interpretations of Trauma: The U.S. Circuit Court of Appeals and Gender-Based Asylum Claims
by
Connie Oxford
Trauma Care 2024, 4(2), 120-147; https://doi.org/10.3390/traumacare4020011 - 16 Apr 2024
Abstract
►▼
Show Figures
This article is based on exploratory research on how the U.S. Circuit Court of Appeals uses the language of trauma in gender-based asylum claims. Gender-based asylum claims include female genital mutilation (FGM), coercive population control (CPC) in the form of forced abortions and
[...] Read more.
This article is based on exploratory research on how the U.S. Circuit Court of Appeals uses the language of trauma in gender-based asylum claims. Gender-based asylum claims include female genital mutilation (FGM), coercive population control (CPC) in the form of forced abortions and forced sterilizations, rape, forced marriage, and domestic violence. The Circuit Courts have reviewed appeals from petitioners with asylum claims since 1946, yet the language of trauma did not appear in the Court’s decisions until 1983. From 1983 to 2023, only 385, 3.85% or less, of the over 10,000 asylum cases before the Circuit Courts used the language of trauma in its legal interpretation of persecution. I have identified 101 gender-based asylum cases that were reviewed by one of the eleven U.S. Circuit Court of Appeals that apply the language of trauma in its legal interpretation of persecution for this analysis. The research question guiding this study is: how does the U.S. Circuit Court of Appeals use the language of trauma when reviewing gender-based asylum cases? This study found that U.S. Circuit Courts use the language of trauma in four ways: precedent cases, policies and reports, physical trauma, and psychological trauma when reviewing gender-based asylum claims. This study provides the first data set of gender-based asylum claims under review at the U.S. Circuit Court of Appeals that use the language of trauma.
Full article
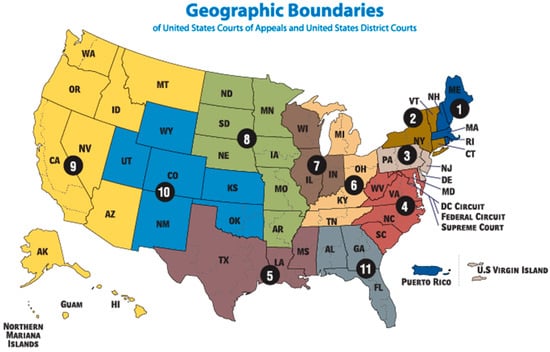
Figure 1
Open AccessReview
The Role of Language Barriers on Hospital Outcomes in Culturally and Linguistically Diverse Patients following Trauma Admission
by
Khang Duy Ricky Le, Kelvin Le, Abdullah Shahzad and Su Jin Lee
Trauma Care 2024, 4(2), 107-119; https://doi.org/10.3390/traumacare4020010 - 6 Apr 2024
Abstract
►▼
Show Figures
(1) Background: Patients who experience acute traumatic injury requiring hospitalisation represent a vulnerable population. The trauma patient often experiences multi-system injuries and complex physiology. Additionally, there are complex socio-ecological issues that impact the care and outcomes of trauma patients. Of interest, culturally and
[...] Read more.
(1) Background: Patients who experience acute traumatic injury requiring hospitalisation represent a vulnerable population. The trauma patient often experiences multi-system injuries and complex physiology. Additionally, there are complex socio-ecological issues that impact the care and outcomes of trauma patients. Of interest, culturally and linguistically diverse populations with language barriers experience worse outcomes in trauma settings. This scoping review evaluates the current evidence on language barriers in this population and the influences on outcomes for trauma patients. (2) Methods: A scoping review was performed following a computer-assisted search of the Medline, Embase and Cochrane Central databases. Papers that evaluated the impact of the language barrier in culturally and linguistically diverse populations and outcomes in acute trauma settings were included. (3) Results: A literature search identified eight articles that were eligible for inclusion. Overall, there was no robust evidence to suggest that such populations were disadvantaged in terms of length of hospital stay and overall mortality. However, studies did identify that these populations were at higher risk of disability and poor mental health outcomes, experienced communication barriers more often and had lower social functioning. (4) Conclusions: This scoping review demonstrates that individuals admitted due to trauma who are from culturally and linguistically diverse backgrounds experience more significant disadvantages concerning psychological and functional outcomes. It is posited this is due to their inability to communicate their complex needs in trauma, however more robust and rigorous research is required to better characterise this effect.
Full article
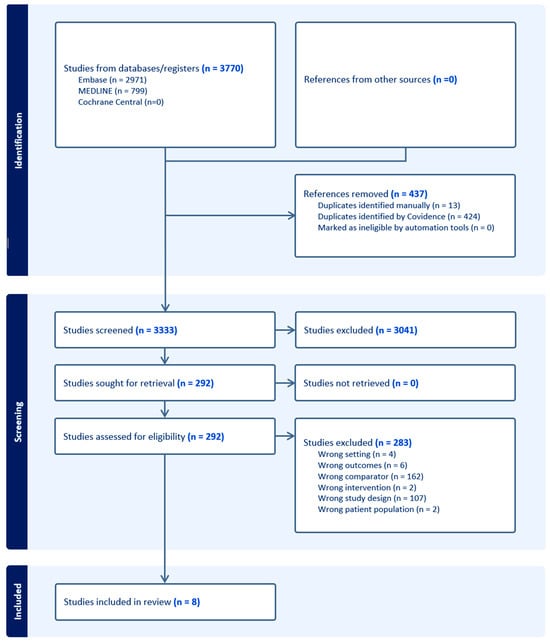
Figure 1
Open AccessArticle
Single-Dose First-Generation Cephalosporin for Extremity Gunshot Wounds Offers Sufficient Infection Prophylaxis
by
Shefali R. Bijwadia, Ilexa R. Flagstad, Margaret A. Sinkler, Samuel T. Davidson, Sandy Vang, Heather A. Vallier and Mai P. Nguyen
Trauma Care 2024, 4(2), 98-106; https://doi.org/10.3390/traumacare4020009 - 3 Apr 2024
Abstract
Antibiotic prophylaxis for extremity gunshot wounds (GSWs) is highly variable. The objective of the present study is to quantify the adherence rate to a protocol for single-dose cephalosporin prophylaxis for extremity GSWs and the impacts on post-injury infection rates. We reviewed patients presenting
[...] Read more.
Antibiotic prophylaxis for extremity gunshot wounds (GSWs) is highly variable. The objective of the present study is to quantify the adherence rate to a protocol for single-dose cephalosporin prophylaxis for extremity GSWs and the impacts on post-injury infection rates. We reviewed patients presenting to a level 1 trauma center with an extremity gunshot wound between 2019 and 2021. Infection rates were compared for patients following the protocol or not, and for patients presenting before or after the protocol’s implementation. Overall, 94% of patients received antibiotic treatment at presentation, but only 34% followed the single-dose antibiotic protocol. The rate of protocol adherence increased from 15% to 39% after the protocol was implemented in the hospital in January 2020 (p = 0.081). Infection rates were not different before and after the protocol implementation (25% vs. 18%, p = 0.45). Infection rates were also not different between patients who did and did not follow the protocol (15% vs. 20%, p = 0.52). The implementation of a single-dose cephalosporin protocol increased adherence to the protocol in a level 1 trauma center without increasing infection rates. These findings support conservative treatment along with a single dose of first-generation cephalosporin antibiotic for uncomplicated extremity GSWs in order to decrease healthcare costs without compromising infection risk.
Full article
Open AccessArticle
Quality of Life in Posttraumatic Stress Disorder: The Role of Posttraumatic Anhedonia and Depressive Symptoms in a Treatment-Seeking Community Sample
by
Craig R. Miller, James E. McDonald, Peter P. Grau and Chad T. Wetterneck
Trauma Care 2024, 4(1), 87-97; https://doi.org/10.3390/traumacare4010008 - 20 Mar 2024
Abstract
Posttraumatic stress disorder (PTSD) is associated with functional impairment and poor quality of life (QoL) across multiple domains, such as social functioning, occupational and educational attainment, physical health, and overall life satisfaction and wellbeing. Yet, there is limited evidence for which PTSD symptom
[...] Read more.
Posttraumatic stress disorder (PTSD) is associated with functional impairment and poor quality of life (QoL) across multiple domains, such as social functioning, occupational and educational attainment, physical health, and overall life satisfaction and wellbeing. Yet, there is limited evidence for which PTSD symptom clusters may be more strongly associated with functional impairment and decreased QoL. We used a seven-factor model of PTSD (re-experiencing, avoidance, negative alterations, anhedonia, externalizing, dysphoric arousal, and anxious arousal) to predict QoL using a latent regression model in a sample (N = 537) of adult patients participating in exposure-based PTSD partial hospitalization programs (PHP). QoL was measured by the Quality-of-Life Satisfaction Questionnaire—Short Form (Q-LES-Q-SF). Among posttraumatic symptoms, anhedonia emerged as the only significant predictor in the model (β = −8.60, SE = 3.02, p = 0.004), when controlling for depression scores. The overall model accounted for 40% of the variance in QoL. Depression was also significantly associated with QoL (β = −1.67, SE = 0.15, p < 0.001), controlling for PTSD symptoms. Our findings are congruent with prior research supporting the role of anhedonia and emotional numbing in functional impairment, yet differ in that other factors of PTSD (e.g., re-experiencing, avoidance, negative alterations) were not significant. Understanding which PTSD symptom clusters are more strongly associated with QoL may inform treatment approaches or allow clinicians to tailor treatments. We discuss implications for treatment and future research.
Full article
Open AccessArticle
Pilot Study of a Resiliency Based and Trauma Informed Intervention for Veterans
by
Kelly Baek, Kimberly R. Freeman, Sophia Truong, Christi Bell and Susanne B. Montgomery
Trauma Care 2024, 4(1), 75-86; https://doi.org/10.3390/traumacare4010007 - 6 Mar 2024
Abstract
►▼
Show Figures
Over 50% of the 21 million veterans in the U.S. with behavioral health challenges are not having their needs met due to stigma and other barriers to care. Resiliency-based models focused on strengthening protective factors to help individuals adapt to adversity in community-based
[...] Read more.
Over 50% of the 21 million veterans in the U.S. with behavioral health challenges are not having their needs met due to stigma and other barriers to care. Resiliency-based models focused on strengthening protective factors to help individuals adapt to adversity in community-based settings, that can be delivered by trained lay persons, are emerging approaches to help address this issue. This longitudinal pilot study evaluated the impact of one such evidenced-based intervention, the Community Resiliency Model (CRM), on veterans’ behavioral health and daily functioning. A sample of 46 English-speaking, ethnically diverse veterans were recruited for this study. Repeated measure analyses showed that CRM skills significantly decreased distress and increased well-being. We also found strong short-term results for measures of daily functioning with a significant longer-term impact on participants’ ability to control their feelings of being ‘amped up’. Most (82%) participants maintained and continued to use the CRM skills daily to weekly and had very positive reactions to the program. Across our analyses, the results of this pilot study suggest that providing CRM trainings to veterans is a feasible, efficacious, and well-received approach to help address much-needed veteran behavioral health.
Full article
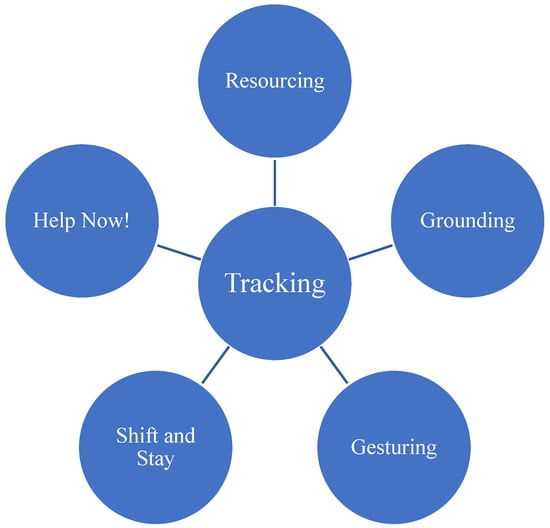
Figure 1
Open AccessArticle
A Mixed-Methods Exploration of Legal Vulnerability, Trauma, and Psychological Wellbeing in Immigrant Caregivers and Youth
by
Regina Roberg, Tamara Camargo and Amy K. Marks
Trauma Care 2024, 4(1), 60-74; https://doi.org/10.3390/traumacare4010006 - 3 Mar 2024
Abstract
(1) Background: Immigrant families in the U.S. face a myriad of migration-related stressors and trauma, and legal vulnerability can further compound such stressors, influencing both immigrant caregiver and child wellbeing. This study explored the relationships between legal vulnerability, trauma, and migration and their
[...] Read more.
(1) Background: Immigrant families in the U.S. face a myriad of migration-related stressors and trauma, and legal vulnerability can further compound such stressors, influencing both immigrant caregiver and child wellbeing. This study explored the relationships between legal vulnerability, trauma, and migration and their effects on caregiving, psychological distress, and resilience in immigrant families. (2) Methods: In total, 37 Latinx immigrant caregiver–child dyads from a community sample were interviewed and completed self-report measures on their experiences of migration, trauma, psychological functioning, and parent–child relationships. (3) Results: Using a community-based, sequential quantitative-qualitative design, person-centered analyses revealed two caregiver clusters: “Personalizing Stress” and “Meaning-making”. Exemplar case analyses characterized differences between clusters, particularly related to trauma symptoms, in which the “meaning-making” cluster endorsed higher levels of psychological functioning and wellbeing compared to the “personalizing stress” cluster, in which the process of creating meaning from adversity appeared to function as a resilience resource for the “meaning-making” cluster. While most indicators of caregiver–child wellbeing were not correlated, family legal vulnerability was strongly correlated with high resilience in children. (4) Conclusions: Clinicians should attend to the resilience resources that immigrant families from legally vulnerable communities utilize, including meaning-making.
Full article
Open AccessArticle
The Influence of COVID-19 on Patient Mobilization and Injury Attributes in the ICU: A Retrospective Analysis of a Level II Trauma Center
by
Yelissa Navarro, Elizabeth Huang, Chandler Johnson, Forrest Clark, Samuel Coppola, Suraj Modi, Gordon L. Warren and Jarrod A. Call
Trauma Care 2024, 4(1), 44-59; https://doi.org/10.3390/traumacare4010005 - 7 Feb 2024
Abstract
►▼
Show Figures
The objectives of this study were to determine the effect of COVID-19 on physical therapy (PT) mobilization of trauma patients and to determine if mobilization affected patient course in the ICU. This retrospective study included patients who were admitted to the ICU of
[...] Read more.
The objectives of this study were to determine the effect of COVID-19 on physical therapy (PT) mobilization of trauma patients and to determine if mobilization affected patient course in the ICU. This retrospective study included patients who were admitted to the ICU of a level II trauma center. The patients were divided into two groups, i.e., those admitted before (n = 378) and after (n = 499) 1 April 2020 when Georgia’s COVID-19 shelter-in-place order was mandated. The two groups were contrasted on nominal and ratio variables using Chi-square and Student’s t-tests. A secondary analysis focused specifically on the after-COVID patients examined the extent to which mobilization (n = 328) or lack of mobilization (n = 171) influenced ICU outcomes (e.g., mortality, readmission). The two groups were contrasted on nominal and ratio variables using Chi-square and Student’s t-tests. The after-COVID patients had higher injury severity as a greater proportion was classified as severely injured (i.e., >15 on Injury Severity Score) compared to the before-COVID patients. After-COVID patients also had a greater cumulative number of comorbidities and experienced greater complications in the ICU. Despite this, there was no difference between patients in receiving a PT consultation or days to mobilization. Within the after-COVID cohort, those who were mobilized were older, had greater Glasgow Coma Scale scores, had longer total hospital days, and had a lesser mortality rate, and a higher proportion were female. Despite shifting patient injury attributes post-COVID-19, a communicable disease, mobilization care remained consistent and effective.
Full article
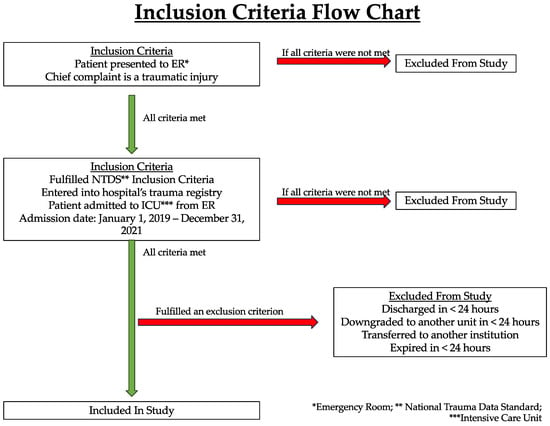
Figure 1
Open AccessReview
Machine Learning in Neuroimaging of Traumatic Brain Injury: Current Landscape, Research Gaps, and Future Directions
by
Kevin Pierre, Jordan Turetsky, Abheek Raviprasad, Seyedeh Mehrsa Sadat Razavi, Michael Mathelier, Anjali Patel and Brandon Lucke-Wold
Trauma Care 2024, 4(1), 31-43; https://doi.org/10.3390/traumacare4010004 - 29 Jan 2024
Abstract
►▼
Show Figures
In this narrative review, we explore the evolving role of machine learning (ML) in the diagnosis, prognosis, and clinical management of traumatic brain injury (TBI). The increasing prevalence of TBI necessitates advanced techniques for timely and accurate diagnosis, and ML offers promising tools
[...] Read more.
In this narrative review, we explore the evolving role of machine learning (ML) in the diagnosis, prognosis, and clinical management of traumatic brain injury (TBI). The increasing prevalence of TBI necessitates advanced techniques for timely and accurate diagnosis, and ML offers promising tools to meet this challenge. Current research predominantly focuses on integrating clinical data, patient demographics, lab results, and imaging findings, but there remains a gap in fully harnessing the potential of image features. While advancements have been made in areas such as subdural hematoma segmentation and prognosis prediction, the translation of these techniques into clinical practice is still in its infancy. This is further compounded by challenges related to data privacy, clinician trust, and the interoperability of various health systems. Despite these hurdles, FDA-approved ML applications for TBI and their subsequent promising results underscore the potential of ML in revolutionizing TBI care. This review concludes by emphasizing the importance of bridging the gap between theoretical research and real-world clinical application and the necessity of addressing the ethical and privacy implications of integrating ML into healthcare.
Full article
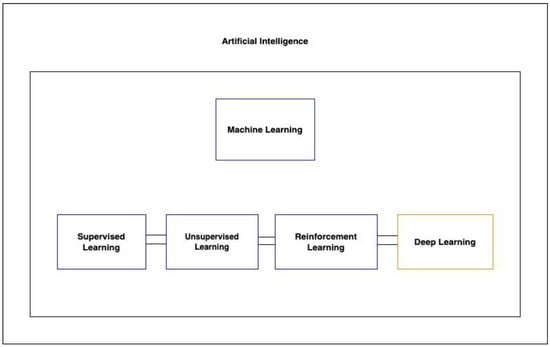
Figure 1
Open AccessBrief Report
Applying and Extending the Conservation of Resources (COR) Model to Trauma in U.S. Veterans
by
Andrea Munoz, Samuel Girguis, Loren Martin and Michael Hollifield
Trauma Care 2024, 4(1), 22-30; https://doi.org/10.3390/traumacare4010003 - 25 Jan 2024
Abstract
►▼
Show Figures
This was a novel pilot study about the relationship between PTSD severity and resource gain and loss using the conservation of resources (COR) model with U.S. Veterans. Higher PTSD severity was predicted to be associated with greater resource loss scores, and lower PTSD
[...] Read more.
This was a novel pilot study about the relationship between PTSD severity and resource gain and loss using the conservation of resources (COR) model with U.S. Veterans. Higher PTSD severity was predicted to be associated with greater resource loss scores, and lower PTSD scores were predicted to be associated with greater resource gain scores. The sample size was limited (N = 19) due to the COVID-19 outbreak. Veterans completed a demographic questionnaire, the Montreal Cognitive Assessment (MoCA), the Combat Exposure Scale (CES), the PTSD Symptom Scale–Interview (PSS-I), the Conservation of Resources–Evaluation (COR-E), and two additional open-ended questions. A statistically significant negative medium effect size was found between PTSD diagnosis and resource gain (r(17) = −0.42, p = 0.039, one-tailed). A large effect size in resource gain scores between PTSD and non-PTSD groups was also found (t(17) = 1.880, p = 0.077, d = 0.87), with the non-PTSD group reporting more gain of resources than the PTSD group. Post hoc tests revealed that the resource gain score of the mild PTSD group was significantly higher than that of the severe + very severe PTSD group (p = 0.034). Results suggest that resource gain, when compared to resource loss, was the strongest predictor for a non-PTSD diagnosis.
Full article
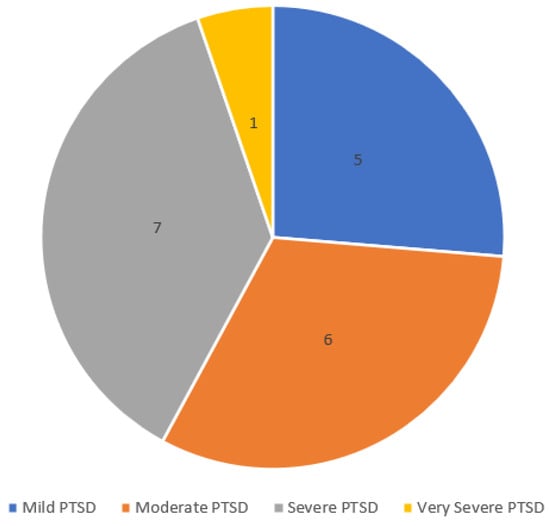
Figure 1
Open AccessArticle
Post-Traumatic Stress Disorder and Blast Exposure in Active-Duty Military Service Members
by
Angela Sekely, Hinza B. Malik, Kayla B. Miller, Yishi Wang and Antonio E. Puente
Trauma Care 2024, 4(1), 10-21; https://doi.org/10.3390/traumacare4010002 - 21 Jan 2024
Abstract
►▼
Show Figures
Objective: Active-duty military personnel in the current wars have experienced unique stressors that deviate from standard PTSD assessment and diagnosis. This situation calls for a refinement of military-related PTSD assessment. To this end, this study assessed the utility of the Trauma Symptom Inventory
[...] Read more.
Objective: Active-duty military personnel in the current wars have experienced unique stressors that deviate from standard PTSD assessment and diagnosis. This situation calls for a refinement of military-related PTSD assessment. To this end, this study assessed the utility of the Trauma Symptom Inventory (TSI) in diagnosing PTSD among active-duty military personnel. The past literature has validated the TSI using populations with a small sample size. Hence, this study aimed to fill the gap by using a large sample size of 670 military members to examine whether the TSI is useful for military populations. Setting: Participants were referred to Carolina Psychological Health Services, in Jacksonville, North Carolina by military neurologists and other qualified medical officers from the Naval Hospital in Camp Lejeune, a military base located in Jacksonville, NC, for neuropsychological evaluation due to reported cognitive deficits related to military deployment (i.e., head injury due to exposure to blast injuries). Participants: Based on clinical diagnosis, comprehensive neuropsychological testing, and self-reported data, personnel were classified into four groups: blast exposure (n = 157), PTSD diagnosis (n = 90), both blast exposure and PTSD (n = 283), and neither blast exposure nor PTSD (n = 140), which helps provide a comprehensive picture of the utility of the TSI. Results: The TSI’s 10 clinical scales could distinguish between all groups. Discriminant function analysis showed that an optimally weighted combination of scales correctly predicted 66.67% of PTSD-positive cases and 35.11% of PTSD-negative cases. Conclusion: These findings provide support for the use of the TSI in the assessment of PTSD in active-duty military personnel. Due to the release of TSI-2, there is a need to replicate this data. However, the validity data has indicated a high concordance between the TSI and TSI-2, bolstering confidence in the current findings of the study.
Full article
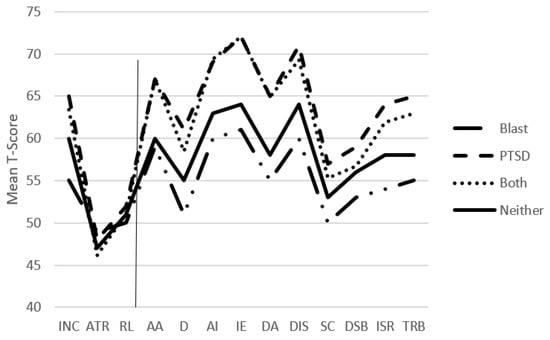
Figure 1
Open AccessBrief Report
A Comparative Gender Analysis of Injury Characteristics, Treatments and Outcomes among Persons Seeking Emergency Care in Kigali, Rwanda
by
Lise Mumporeze, Chantal Uwamahoro, Doris Uwamahoro, Aly Beeman, Destry Jensen, Oliver Young Tang, Enyonam Odoom, Spandana Jarmale, Stephanie C. Garbern, Catalina González Marqués, Andrew Stephen and Adam R. Aluisio
Trauma Care 2024, 4(1), 1-9; https://doi.org/10.3390/traumacare4010001 - 19 Dec 2023
Abstract
In high-income nations, gender has been associated with injury characteristics. This study evaluated injury epidemiology and care based on gender at the Centre Hospitalier Universitaire de Kigali in Rwanda. Patients presenting to the emergency department with acute injuries were prospectively enrolled from 27
[...] Read more.
In high-income nations, gender has been associated with injury characteristics. This study evaluated injury epidemiology and care based on gender at the Centre Hospitalier Universitaire de Kigali in Rwanda. Patients presenting to the emergency department with acute injuries were prospectively enrolled from 27 January–28 June 2020, and descriptive statistics were performed with comparisons between males and females. Of 601 patients, 25.6% were female and 74.4% were male. There were gender differences in the mechanism of injury, with females more likely to be injured in falls (43.5% versus 23.0%, p = 0.001); meanwhile, males were more likely to suffer road traffic accidents (52.6% versus 39.6%, p = 0.006). The severity of injury was similar between genders based on the mean Kampala Trauma Score (14.4 versus 14.7, p = 0.09). Females were more likely to have been transported by prehospital services (87.7% versus 72.9%, p = 0.001), and less likely to receive acute treatment during the first six hours of care (67.5% versus 78.1%, p = 0.009). There was no significant difference in mortality between females and males (2.0% versus 1.3%, p = 0.568). This study highlights differences in the epidemiology and care between males and females presenting for emergency injury care in Rwanda. These findings can inform future research and developments in gender-centered healthcare delivery.
Full article
Open AccessReview
Exploring the Increased Risk of Post-Traumatic Stress Following a Sexual Assault: Implications for Individuals Who Identify as a Sexual Minority
by
Jodie Murphy-Oikonen, Jo-Ann Vis and Rachel Egan
Trauma Care 2023, 3(4), 352-361; https://doi.org/10.3390/traumacare3040029 - 17 Dec 2023
Abstract
Decades of research have enhanced our understanding of the psychological impact of sexual victimization, including risk factors through which post-traumatic stress disorder (PTSD) manifests. Research on sexual assault and PTSD predominately reflects the experience of heterosexual women, yet sexual minorities are both at
[...] Read more.
Decades of research have enhanced our understanding of the psychological impact of sexual victimization, including risk factors through which post-traumatic stress disorder (PTSD) manifests. Research on sexual assault and PTSD predominately reflects the experience of heterosexual women, yet sexual minorities are both at increased risk of sexual assault and suffer greater negative health outcomes from it. In these cases, PTSD is linked to a clearly identifiable cause, thereby making it possible to identify individuals at risk, enhance interventions immediately following the traumatic event, and offer services to mitigate further harm. This narrative review explores the potential risk factors for PTSS and PTSD among individuals who experience sexual assault and identify as a sexual minority. Knowledge of these compounding risk factors among service providers will assist in obtaining sexual assault disclosures in a sensitive and supportive manner, leading to the provision of early interventions to mitigate the risks of developing PTSD following sexual assault. The findings suggest that empirical investigation is urgently required to develop evidence-informed practices in providing targeted interventions for sexual and gender minorities following a sexual assault and mitigating further adverse health outcomes.
Full article
Open AccessArticle
Raising Voice at School: Preliminary Effectiveness and Community Experience of Culture and Practice at an Australian Trauma-Responsive Specialist School
by
Julie C. Avery, Emma Galvin, Joanne Deppeler, Helen Skouteris, Justin Roberts and Heather Morris
Trauma Care 2023, 3(4), 331-351; https://doi.org/10.3390/traumacare3040028 - 16 Dec 2023
Cited by 1
Abstract
►▼
Show Figures
The aim of this study is three-fold: (1) to explore multiple community member views of core elements of trauma-responsive practice at a specialist school; (2) to explore impact on student wellbeing and learning outcomes, and educator experiences of their workplace; and (3) to
[...] Read more.
The aim of this study is three-fold: (1) to explore multiple community member views of core elements of trauma-responsive practice at a specialist school; (2) to explore impact on student wellbeing and learning outcomes, and educator experiences of their workplace; and (3) to explore insights into implementation challenges and enablers. This study uniquely incorporates four participant cohorts: parents or caregivers, educators, and community agencies involved with school students and their families. It utilises a mixed-methods approach with an emphasis on the voice of participants and their lived experience of a trauma-responsive specialist school. The data identify a trauma-responsive school culture, high staff satisfaction, improved student wellbeing and attendance, and progress towards learning goals. Reflective analytic themes centre on a collective experience of the school as a connected community, emphasising relationships, safety, collaboration, mutuality, voice, and empowerment. Findings show that the practices most valued across the cohorts centre on the collective experience of the school as a connected community, emphasising relationships, safety, deep listening, collaboration, mutuality, voice, and empowerment. Trauma-informed principles frame the discussion and implications for equity-focused trauma-responsive practice and policy development. Implications for practice and policy development are discussed.
Full article
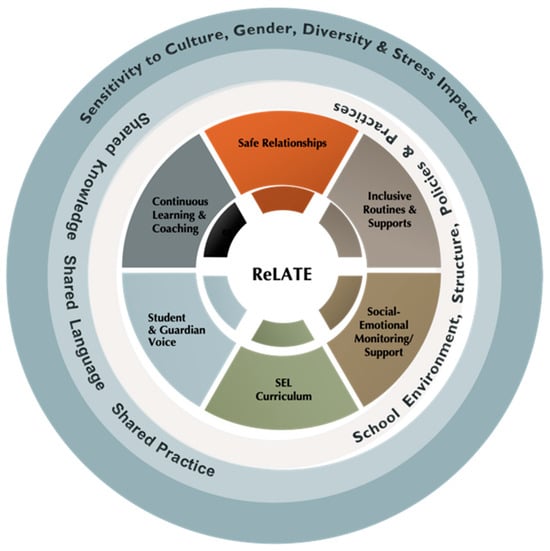
Figure 1
Open AccessArticle
The Effect of Fracture Type on Restoration of Radiographic Parameters and Early Loss of Reduction in Surgical Treated Distal Radius Fractures
by
Varun Sambhariya, Tyler Roberts, Colin Ly, Alison Ho and William F. Pientka II
Trauma Care 2023, 3(4), 321-330; https://doi.org/10.3390/traumacare3040027 - 4 Dec 2023
Abstract
Purpose: Early loss of reduction remains a challenging complication in distal radius fracture management. There are limited data on factors that correlate with early loss of reduction. The Arbeitsgemeinschaft für Osteosynthesefragen (AO) classification has become a popular way of evaluating complex fracture patterns.
[...] Read more.
Purpose: Early loss of reduction remains a challenging complication in distal radius fracture management. There are limited data on factors that correlate with early loss of reduction. The Arbeitsgemeinschaft für Osteosynthesefragen (AO) classification has become a popular way of evaluating complex fracture patterns. This study aims to determine the impact of fracture pattern, as determined by the AO classification, on restoration of intraoperative parameters, early loss of reduction, and time to fracture union in operatively treated distal radius fractures. Methods: Following IRB approval, adult patients with surgically treated acute distal radius fractures at a single level I institution were identified. Retrospective chart and radiographic review were used to obtain AO classification, postoperative radiographic parameters, early loss of reduction, time to fracture union, as well as any complications. Results: 422 patients with operatively treated distal radius fractures were included in this study. Across fracture patterns, there were no significant differences in restoration of radial height or inclination. Higher severity fracture classifications had decreased restoration of volar tilt. Overall, simple fractures (A2, C1) and partial articular fractures (B1, B2, B3) had higher rates of satisfactory alignment restoration compared to comminuted fractures (A3, C2, C3). Although there were differences in restoration of radiographic parameters, fracture type did not correlate with loss of reduction within 30 days. C type fractures correlated with increased weeks to radiographic healing. Conclusions: This study establishes that distal radius fracture pattern, as determined by the AO classification, has a significant impact on intraoperative restoration of parameters but does not correlate with early loss of reduction. Furthermore, more difficult fracture patterns may have a longer time to fracture union, but fracture type does not appear to have an effect on postoperative complications.
Full article
Open AccessArticle
Assessing Risk Factors for Victims of Violence in a Hospital-Based Violence Intervention Program
by
Gaylene Armstrong, Taylor Gonzales, Michael R. Visenio, Ashley A. Farrens, Hannah Nelson, Charity H. Evans, Jennifer Burt, Zachary M. Bauman, Mark Foxall and Ashley A. Raposo-Hadley
Trauma Care 2023, 3(4), 308-320; https://doi.org/10.3390/traumacare3040026 - 11 Nov 2023
Abstract
Introduction: Personal, behavioral, and environmental risk factors are correlated to varying degrees with each other and with the overall likelihood of violent reinjury. When used with fidelity, risk assessment instruments, including the violence reinjury risk assessment instrument (VRRAI), identify domains in which individuals
[...] Read more.
Introduction: Personal, behavioral, and environmental risk factors are correlated to varying degrees with each other and with the overall likelihood of violent reinjury. When used with fidelity, risk assessment instruments, including the violence reinjury risk assessment instrument (VRRAI), identify domains in which individuals present elevated risk levels to aid in matching services with needs. Less is known about the collinearity among risk factors for violently injured individuals admitted to hospitals. Collinearity between risk factors has ramifications for predictive modeling of violent reinjury risk. The objective of this study was to identify significantly correlated risk factors when the VRRAI was used by hospital-based violence intervention programs (HVIP) for clients. Materials and Methods: Victims of violent injury by modality of firearm, stabbing, and physical assault who were admitted to a level 1 trauma center at a single institution were voluntarily enrolled in a hospital-based violence intervention program (HVIP) between September 2020 and June 2022. Violence intervention specialists (VIS) completed the VRRAI within the first month of participant enrollment. The VRRAI is comprised of 29 binary indicators that may signal elevated risk of violent reinjury. Data from completed assessments were used to apply risk-need-responsivity (RNR) principles along with phi coefficients of key indicators to examine overlap and prevalence in the population. Results: A total of 98 participants were enrolled in the HVIP. The median age was 27 years old and 79 (80.6%) were male, while 66 (67.3%) were non-Hispanic Black or African American, 9 (9.2%) were non-Hispanic White, and 17 (17.3%) identified as Hispanic or Latino. Several statistically significant relationships existed between key risk indicators in the VRRAI. Importantly, a robust relationship was found between the two dynamic risk factors of having heavy connection with gangs and a perception of imminent threat of violence (φc = 0.57, p < 0.01). Conclusion: Data suggest that some variables could be consolidated or removed from the VRRAI to create an even shorter instrument that can be performed more rapidly in the clinical setting. The application of the RNR model illustrates a limited number of dynamic risk factors that could be immediately addressed as part of case management should be prioritized among the questions selected from the VRRAI for inquiry at the intake assessment.
Full article
Open AccessSystematic Review
Does a Preoperative Carbohydrate Drink Reduce Postoperative Inflammation? A Systematic Review and Meta-Analysis
by
Khasim Zakaria Haider and Zubair Ahmed
Trauma Care 2023, 3(4), 294-307; https://doi.org/10.3390/traumacare3040025 - 9 Nov 2023
Abstract
►▼
Show Figures
Since 1995, it has been known that carbohydrate drinks (CHDs) can be safely consumed two to three hours (2–3 h) preoperatively. Furthermore, preoperative CHDs significantly benefit many outcomes, such as thirst, hunger, and insulin resistance. Patients, however, still fast excessively. This study aimed
[...] Read more.
Since 1995, it has been known that carbohydrate drinks (CHDs) can be safely consumed two to three hours (2–3 h) preoperatively. Furthermore, preoperative CHDs significantly benefit many outcomes, such as thirst, hunger, and insulin resistance. Patients, however, still fast excessively. This study aimed to determine if a CHD, consumed 2–3 h preoperatively, impacts postoperative inflammation compared to a placebo drink or fasting. This was achieved through analysing the levels of interleukin-6, C-reactive peptide, and serum albumin 10–24 h postoperatively. We conducted a systematic review of randomised control trials. We comprehensively searched the Embase, MEDLINE and Web of Science databases, identified 473 studies, and, after screening, were left with 10 randomised control trials. Our meta-analyses found a significantly lower mean interleukin-6 level of −21.26 pg/mL ((95% CI −33.37, −9.15); p = 0.0006) postoperatively in patients given a preoperative CHD compared to fasting and a significantly higher mean serum albumin level of 2.56 g/L ((95% CI 1.41, 3.71); p < 0.0001) postoperatively in patients given a preoperative CHD compared to a placebo. Our results therefore show that a CHD, consumed 2–3 h preoperatively, lowers proinflammatory cytokine levels and increases serum albumin levels. Thus, our study reinforces guideline recommendations to give patients a CHD 2–3 h preoperatively for improved outcomes.
Full article
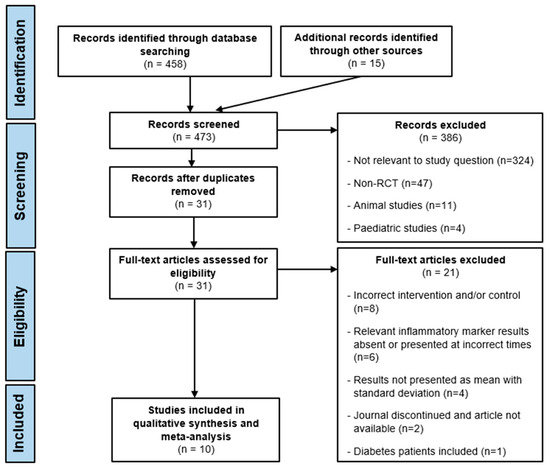
Figure 1
Open AccessReview
Addressing Attrition from Psychotherapy for PTSD in the U.S. Department of Veterans Affairs
by
Alexander J. Lee and Lucas S. LaFreniere
Trauma Care 2023, 3(4), 274-293; https://doi.org/10.3390/traumacare3040024 - 8 Nov 2023
Abstract
The United States Department of Veterans Affairs (VA) uses a systematized approach for disseminating evidence-based, trauma-focused psychotherapies for post-traumatic stress disorder (PTSD). Within this approach, veterans with PTSD must often choose between Prolonged Exposure (PE) and Cognitive Processing Therapy (CPT), each delivered in
[...] Read more.
The United States Department of Veterans Affairs (VA) uses a systematized approach for disseminating evidence-based, trauma-focused psychotherapies for post-traumatic stress disorder (PTSD). Within this approach, veterans with PTSD must often choose between Prolonged Exposure (PE) and Cognitive Processing Therapy (CPT), each delivered in their standard protocols. Many veterans have been greatly helped by this approach. Yet limiting trauma-focused therapy to these two options leaves the VA unable to fully address the needs of a variety of veterans. This limitation, among other factors, contributes to the suboptimal attrition rates within the VA. The present review proposes solutions to address treatment barriers that are both practical (such as time and travel constraints) and psychological (such as resistance to trauma exposure). By reducing barriers, attrition may lessen. Proposed countermeasures against practical barriers include intensive protocols, shortened sessions, telehealth, smartphone application delivery, or any combination of these methods. Countermeasures against psychological barriers include alternative evidence-based treatment programs (such as Acceptance and Commitment Therapy), intensive protocols for exposure-based treatments, and the integration of components from complementary treatments to facilitate PE and CPT (such as Motivational Interviewing or family therapy). By further tailoring treatment to veterans’ diverse needs, these additions may reduce attrition in VA services for PTSD.
Full article
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Healthcare, IJERPH, Nursing Reports, Trauma Care, Hospitals
Integrated Health Services across Different Levels: Worldwide Experiences
Topic Editors: Alexandre Morais Nunes, Diogo Cunha FerreiraDeadline: 28 February 2025

Conferences
Special Issues
Special Issue in
Trauma Care
Psychological and Neurobiological Bases of Threat Processing in Victims of Pandemics and Natural Disasters
Guest Editors: Massimiliano Conson, Laura SaglianoDeadline: 30 June 2025







